It’s hard to imagine a Britain without free healthcare. A country with hospitals all individually run by local councils or charities and general practitioners (GPs) who send you a bill for their services. One in which the poor might not seek treatment for coughs, cholera or cancer due to the potential embarrassment of not being able to pay for it.
Pre-1948 and the vision of Nye Bevan – the trade union leader turned Labour health minister – and this was the sorry state of British healthcare. Bevan pioneered the development of the National Health Service (NHS), the world’s first universal health system free at the point of use. On 5 July 1948 he opened the first NHS hospital in Manchester, describing it as “the most civilised step any country has ever taken”. It has been a great source of pride for Britons ever since.
But almost throughout its existence, the NHS has been plagued with financial difficulties. Just three years after its grand opening, Bevan resigned from government in protest at the introduction of charges for glasses and prescriptions. Complaints about costs and extravagance came thick and fast and many hospitals reported significant waste and misuse.
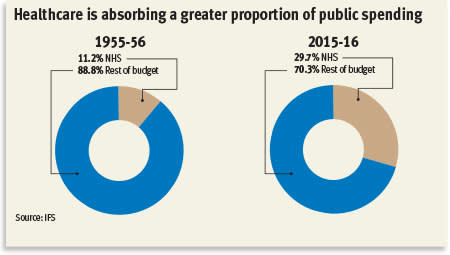
Such concerns have never been far from the NHS and now, almost 70 years on from its launch, those fears carry more weight than ever before. In the year to March 2016 – the last full year of financial results we’ve seen from the NHS following the government’s decision to hold off releasing results until after the general election – healthcare spending in the UK reached £100bn. Even after adjusting for inflation that’s more than 10 times the amount spent in the year the NHS was founded.
The NHS is creaking at the seams. In the 2016 financial year it ran up a £1.85bn deficit and, without the £3bn emergency cash injection from the treasury, that deficit is likely to have been even larger in the year just ended.
The financial strain is showing in the quality of care. More than a tenth of NHS acute specialist trusts are rated inadequate for safety and you have to go back to the summer of 2015 for the last time A&E waiting time targets were met in England. Most worryingly, 3.9m people are currently on the NHS procedure waiting lists and, without a substantial increase in funding, that number is expected to rocket to 5.5m by 2019. In the words of the chief executive of NHS Improvement, Jim Mackey, “the NHS is in a mess”.
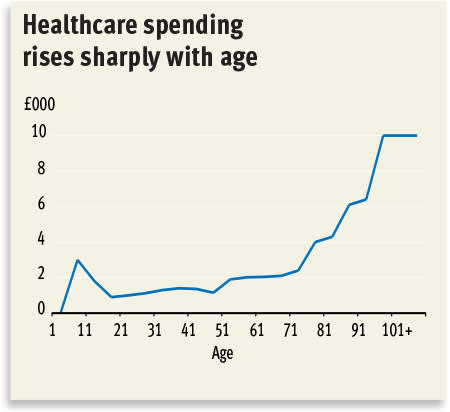
But perhaps we expect too much from our beloved free healthcare system. Today it is serving a population 26 per cent larger than at its origin, life expectancy in the UK is 13 years greater than it was in 1948 and the proportion of our population aged 65 or over is creeping fast towards 20 per cent. And with more elderly, demand is rising for two expensive types of care: looking after the dying and caring for people with more than one chronic illness. According to research from King’s College London, about a quarter of NHS finances are spent on patients who are in the last year of their life. Lifestyle illnesses such as obesity and diabetes are also adding to the demand. Type 2 diabetes is believed to cost the NHS £10.3bn each year, and in the past 10 years the number of diabetics in the UK has risen by 3m.
The NHS is in dire need of more money. In 2013, NHS England and various independent analysts wrote the ‘five-year forward view’, which concluded that the “mismatch between resources and patient needs” would reach nearly £30bn a year by the 2021 financial year.
But while most agree that more funding is key, fewer are willing to pay for it. Polls suggest that only a minority of British people would be willing to pay more in general taxation to pay for the NHS. Moreover, increased spending may not provide the ultimate solution. The Labour party under Gordon Brown increased NHS funding by more than a tenth, but the response was just a 2 per cent increase in productivity.
So, it would appear that higher expenditure alone is not going to save our NHS. Instead the solution lies in efficiency: the NHS must do more with what it already spends. A topic clouded by politics, finding a solution to this conundrum is no simple task. That said, stripping out the political implications, the independent sector has the potential to be a force for good in healthcare in the UK.
1. Workforce worries
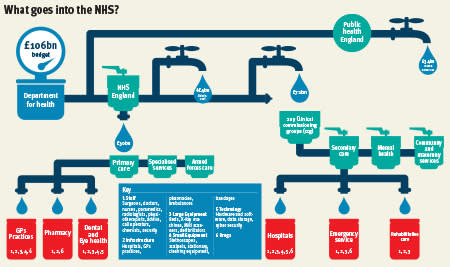
At the last count, staff costs were the single biggest drain on NHS expenses, absorbing two-thirds of hospital budgets in the 2016 financial year. To a certain extent, that’s not surprising. The NHS – with its 1.7m workers – is the fifth-largest employer globally, a league table topped by the US Department for Justice and the Chinese army.
But it is also widely accepted that staffing costs could easily be cut by lowering expenditure on using part-time employee and recruitment companies. That is easier said than done. Filling the staffing requirements of this juggernaut requires extensive use of expensive recruitment agencies – in Greater London alone there are 175 agencies that help with NHS recruitment – which in the 2016 financial year cost £3.6bn.
At present, the largest NHS recruiter is a government-owned organisation that “aims to save trusts up to 20 per cent of their flexible workforce costs”. NHS Professionals was founded in 2001 and turned profitable in 2010, meaning it no longer relies on financial aid from the Treasury. Even so, the government recently made the controversial decision to put the organisation up for sale, with London-listed company Staffline (STAF) expected to be its lucky new owner. Lucky because NHS Professionals has an incredibly stable source of revenue from NHS England and rapidly rising demand, which in 2016 sparked a 10 per cent increase in revenues.
While the Conservative party said selling off NHS Professionals was part of its plan to “maximise the value of assets and commercial opportunities”, it does not seem unfair to question the benefits of privatising this profitable division of British healthcare.
2. Building better infrastructure
In other areas, privatisation – though still controversial – has proved effective. Building, day-to-day running and maintenance of hospital buildings – all highly capital-intensive activities – is being increasingly outsourced to private providers. Independent groups such as Spire Healthcare (SPI) have also reported an increase in the number of patients they treat on behalf of the NHS. Anthony Mannion, director of communications at Spire, thinks that increased use of private providers for non-critical care, such as orthopaedics, will be crucial to the longevity of the NHS.
There have also been calls for consolidation in secondary care facilities across the UK, which are widely considered to be excessive in number. Across the world, hospital providers are scaling up and creating a smaller number of specialist facilities, which has improved health outcomes. For example, when Denmark reduced the number of specialist colorectal-cancer treatment centres, post-operative mortality rates improved by almost two-thirds. In London, fewer people have died of strokes since it merged 32 specialist sites into eight.
It’s a similar story in primary care, where 40 per cent of the UK’s 9,000 GP practices are considered unfit for purpose. The government has promised to up the proportion of healthcare spending in primary care to help create a number of ‘super-practices’, with shared admin and back-office staff. “In the next five to 10 years there will be more changes to primary care than ever before,” said Alan Pennell, finance director of MedicX Fund (MXF), one of three London-listed primary care property investment groups.
The benefits of creating these super-practices are two-fold. As well as lowering staff and admin costs, new GP surgeries are expected to host more facilities to alleviate the demand on emergency care, which costs the NHS about 10 times more than a visit to the GP. MedicX and peers Primary Health Properties (PHP) and Assura (AGR), which own, develop and rent out the land used for primary care facilities, are well placed to benefit from the proposed increase in funding to this area of healthcare.
3. Diagnosing the problem
To a patient, there can surely be no greater demonstration of the inefficiencies of the NHS than a simple blood test. Today, a blood test to check a patient for tonsillitis can require a GP to take the sample, someone to send that sample away for analysis, a large corporation to use its diagnostic machine to examine for illness, someone to send the results back, a secretary to inform the patient that their results are ready and another GP to discuss those results. Point-of-care testing – whereby an easy-to-use, portable machine, can analyse a blood sample in minutes while the patient is still in the surgery – is widely considered one of the most necessary developments for taking costs out of the NHS.
And there are plenty of companies helping to make that possible. Netscientific (NSCI) and Deltex Medical (DEMG) currently provide solutions to monitor blood levels from home, while Toumaz (TMZ) claims its electronic plasters can detect heart attacks. Concepta Diagnostics' (CPT) MyLotus self-testing kit helps women with unexplained infertility conceive. Meanwhile, engineers Carclo (CAR), Morgan Advanced Materials (MGAM), Oxford Instruments (OXIG), Renishaw (RSW) and Victrex (VCT) all manufacture various different forms of sophisticated medical diagnostic equipment.
Genetics is proving just as helpful in diagnostics as it is in the wider medical world. For example, Genedrive (GDR) has developed a molecular diagnostic system which can rapidly analyse a person's genotype to test for infectious diseases. And Oncimmune's (ONC) 'EarlyCDT' scans DNA for signs of lung cancer up to four years before symptoms reveal themselves.
Meanwhile, scanning for illnesses using X-ray or MRI is proving another costly challenge for the NHS, largely due to modern medicine’s increasing reliance on expensive scanners and specialist radiology staff. In 2014, the Royal College of Radiologists proclaimed that “radiology services in the UK are in crisis”. The organisation proposes that existing radiology services should collaborate to form networks of expertise serving a population of several million rather than a few hundred thousand as at present.
There is also an argument for outsourcing radiologist work. Medica (MGP), for example, employs experienced radiologists to remotely assess human body scans for diagnostics purposes and uses its bespoke IT platform to report its findings. Cambridge Community NHS Trust, which uses Medica’s services, says the partnership has “improved the quality of service offered to patients and referrers alike”.
4. Procuring a solution
There is no one description for all the small tools used in healthcare. Will Pressley, the director at Spire’s new Nottingham hospital, refers to all the scalpels, stethoscopes and stationary as the “knives and forks”. Unfortunately, in the NHS, there is also no one organisation in charge of the procurement of the many thousands of pieces of small equipment used by all the hospitals around the UK.
But there could be. NHS Supply Chain used to be a government-owned body and claims to “deliver savings to our customers”. But since the organisation was sold to German group Deutsche Post DHL (DE:DPW), many NHS trusts have been unwilling to use its services. The result is that a huge amount of the small equipment used by hospitals, from little yellow pencils to baked beans in the catering department, are ordered separately by individual hospitals.
Paul Swinney, chief executive of Tristel (TSTL), which supplies the NHS with all the anti-bacterial wipes and foams used in critical care units, called it a “very jumbled-up process”. About 70 per cent of Tristel’s UK orders come from NHS Supply Chain, but the rest is all ordered by individual hospitals, some of which also use the NHS Supply Chain. “You wouldn’t find a private company ordering in such a haphazard way,” said Mr Swinney.
NHS Supply Chain wants to find a solution. Together with the Department of Health it has established a £300m fund to enable the NHS to buy equipment in bulk. The 2013 Carter Review said that £1.2bn could be saved over the next four years if procurement becomes a priority. But hospitals must start using the services of NHS Supply Chain more if the plans are to be effective.
5. Technology troubles
According to Mr Pressley of Spire Nottingham, “everything that goes into a hospital relies on IT in some shape or form”. From managing the temperature and the lighting to performing an MRI scan, technology is one of the most important parts of effective day-to-day running of a hospital.
From a care perspective, the advances in technology are already proving beneficial. For example, the huge amount of data that can be stored and retrieved from the cloud is helping to improve patient diagnostics and treatment. But there is also a massive logistical component to the running of a hospital, which could be improved by investment in technology. And many companies boast the software to make this possible. Ideagen's (IDEA) digital management software is used to create paperless and easier-to-navigate medical records. General practitioners can use EMIS's (EMIS) software to enable them to easily share patient data and individualised care plans in real time. But data sharing must be done with caution as the more intertwined an IT system, the more vulnerable it is to a breach.
The technological vulnerability of the NHS was revealed all too plainly in April when its IT systems were infiltrated by ransomware known as WannaCry. The malicious software, which demanded payment for the release of sensitive documents, had entered the NHS computer systems through its Windows XP software.
But NHS operators had been warned of the dangers of the attack after information about a weakness in the XP software was stolen from the US Department of Justice just one month earlier. According to management at the NHS’s cyber security provider, Sophos (SOPH), Windows had released a free ‘patch’ for the software, which would have prevented the hack from occurring if all of the computers had been updated. Just one weak link in the massive NHS chain of data allowed the software in and, once there, it spread very easily.
The full extent of the costs of this attack are yet to be revealed but, for patients, the impact was clear. Operations and appointments were cancelled and ambulances diverted at up to 40 hospital trusts. Doctors warned that the infiltration could cost lives. In the age of technology criminals, investment in cyber security is of utmost importance.
6. Gold standard of treatment
Arguably the most important things in a hospital – apart from its staff – are the drugs that are going to make patients better. All medicines used in the UK – whether that be NHS or private hospitals – are regulated by the government body NICE. Just having one organisation in charge of approving drugs for the whole country is extremely beneficial as NICE is in a strong position to negotiate fair prices with the drugs companies.
But still, this is an area where greater efficiency can result in cost savings and improved outcomes for patients. For example, the current gold standard of cancer therapy in the UK is chemotherapy, a procedure that leaves a patient with symptoms that are often far worse than the cancer itself. Progress in cancer treatment from companies such as Merck (US:MRK), Bristol-Myers Squibb (US:BMY) and AstraZeneca (AZN) has the potential to enormously reduce the amount of time patients have to spend in hospital, which will subsequently lower the cost of treatment. There is a similar trend in many different illnesses. Verona Pharma's (VER) RPL554 is said to improve treatment for patients with the most severe respiratory conditions, while Premaitha Health (NIPT) is attempting to use maternal blood samples to reduce the risk of babies being born with certain genetic illnesses. BTG's (BTG) entire portfolio of medicines is designed to extract costs from healthcare by moving patients through the system quicker. “No one wants to be in hospital for very long,” says a 78-year-old inpatient at a hospital in Watford. “If better drugs can get me out of here quicker, that’s good news for everyone.”
Don't mention the politics…
Following last week’s general election surprise (or disaster, depending which side of the political spectrum you are on), politics has become an even more uncertain muddle. But, when it comes to healthcare in the UK the topic is difficult to avoid.
The Labour party – which never let up on an opportunity to remind the people that the NHS was its creation – adamantly opposes independent interference in the NHS and believes the best way to deal with its problems is to increase spending through ramping up taxes. The Conservatives on the other hand are keen on privatisation, but their unwillingness to commit fully is arguably leading to even greater costs.
But the bottom line is that the NHS is in crisis and, with the population growing, ageing and getting unhealthier, the demands on it are not likely to let up. No political party has ever dared suggest taking away our beloved NHS, but perhaps, in order to save it from total ruin, now is the time for a healthcare leader to dare to shake things up.